 Causes of Swan Neck Deformity
Causes of Swan Neck Deformity
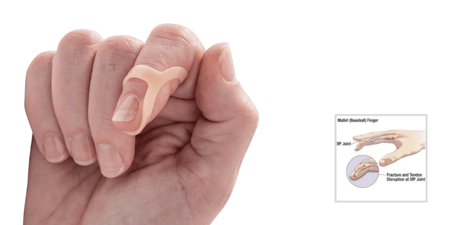
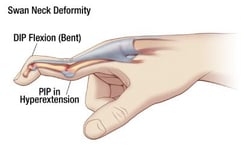
At first glance, diagnosing Swan Neck Deformity seems like a "no brainer". Typically it is a straightforward diagnosis due to its distinct visual characteristics of hyperextension of the proximal interphalangeal (PIP) joint and flexion of the distal interphalangeal (DIP), along with a contorted finger shape resembling that of a swan neck. And more often than not your patient has Rheumatoid Arthritis (RA).
While RA is a major contributing factor to Swan Neck Deformity, there are many other conditions which can cause this condition as well. These include Cerebral Palsy and Lupus; neurological disorders such as Stroke, Parkinson's Disease and Ehlers-Danlos Syndrome all carry potential risk factors too. Furthermore, post-traumatic flexor tendon ruptures or even ischemic injuries may also be responsible for the development of Swan Neck Deformity in some cases.
| Are you a patient or consumer? Click Here to learn more about a swan neck deformity on our consumer site shopoma.com |
Although its a common condition, over time, if left untreated or treated incorrectly, this malformation can become a significant and painful disability as the imbalance between muscles and tendons progresses. Muscles may contract permanently and joint capsules may rupture. The patient can lose the capacity for bending, pinching, gripping, and grasping.
Evaluating Patients for a Swan Neck Deformity
Swan Neck Deformity patients need a careful evaluation to determine the severity and sources of their PIP hyperextension and DIP flexion. For example, is the hyperextension caused by extrinsic extensor tightness? Is the intrinsic tightness caused by spasticity pertaining to CVA or PD? Is the DIP flexion a result of weakened, disrupted, or perhaps a ruptured terminal extensor tendon?
A thorough examination will more precisely define the severity of the deformity, precise alignment issues, and the best means for correcting the mechanics. (See bottom of page for Nalebuff classification.)
Treating Swan Neck Deformity
Particularly with Swan Neck Deformity, proper diagnosis and early intervention are key to successful management and finding the best means of righting the imbalance. Physical and occupational therapy, based on the root cause and severity of the deformity, may include daily massage, stretches, and exercise.
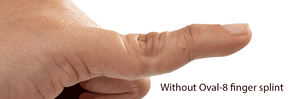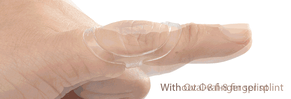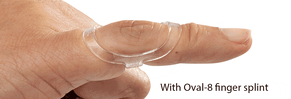
Splints are an integral part of treatment for re-aligning the joints. Oval-8 Finger Splints (available in Classic beige and NEW Oval-8 CLEAR) are often very successful long-term solutions in patients with mild to moderate Swan Neck Deformity. The comfortable, unobtrusive Oval-8's block hyperextension without limiting flexion to keep the finger in proper alignment and prevent hyperextension at the PIP joint. When hyperextension at the PIP joint is controlled, the ability to control motion at the DIP joint is also improved.
With careful adherence to splinting and therapy, most Swan Neck Deformity patients can regain and maintain balance and function in the finger.
In severe cases, surgical options should be considered and may include soft tissue repair, arthroplasty, replacement, or fusion. Splinting is indicated prior to and following surgery.
In 1989, Hand Clinics (Elsevier) published “The rheumatoid swan-neck deformity” by orthopedic surgeon Edward A. Nalebuff, MD, FACS. Today, Dr. Nalebuff’s classification is used to guide the treatment choices for patients with swan neck deformities. Dr. Nalebuff, who received his medical degree from Tufts University School of Medicine in 1953, retired in 2014.
The Nalebuff classification of swan-neck deformities
- Type I - proximal interphalangeal joints are flexible in all positions.
- Type II - proximal interphalangeal joint flexion is limited in certain positions.
- Type III - proximal interphalangeal joint flexion is limited in all positions.
- Type IV - proximal interphalangeal joints are stiff and have a poor radiographic appearance.)